Summary
Objectives:
The objective of this study was to investigate the differences between the results of two serology tests for the detection of COVID-19 among medical personnel, who have a higher risk of infection.
Methods:
Immunochromatography (ICG) rapid test kit and quantitative chemiluminescence immunoassay (CLIA) antibody test were performed. The differences in the prevalence of IgM and IgG antibodies in different serological tests were analyzed descriptively.
What is an immunoglobulin test?
An immunoglobulin (im-yeh-no-GLOB-yeh-len) test measures the level of types of antibodies in the blood. The immune system produces antibodies to protect the body from bacteria, viruses, and allergens. The body makes different antibodies, or immunoglobulins, to fight different things. For example, the chickenpox antibody is not the same as the mononucleosis antibody. Sometimes the body can even mistakenly produce antibodies against itself, treating healthy organs and tissues as foreign invaders. This is called an autoimmune disease.
The types of antibodies are:
- Immunoglobulin A (IgA): Found in the linings of the respiratory tract and digestive system, as well as in saliva (spit), tears, and breast milk.
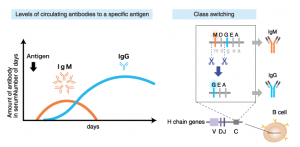
- Immunoglobulin G (IgG): This is the most common antibody. It is in the blood and other body fluids, and it protects against bacterial and viral infections. IgG may take time to form after infection or immunization.
- Immunoglobulin M (IgM): Found primarily in the blood and lymphatic fluid; it is the first antibody the body produces when fighting a new infection.
- Immunoglobulin E (IgE): Normally found in small amounts in the blood. There may be higher amounts when the body overreacts to allergens or is fighting an infection from a parasite.
- Immunoglobulin D (IgD): This is the least known antibody, with only small amounts in the blood.
Why are immunoglobulin tests done?
Doctors can check immunoglobulin levels to see if a person has an infection or is protected from infection (immune to it). Doctors also use immunoglobulin tests to help diagnose immunodeficiencies (when the immune system isn’t working the way it should). Doctors may suspect an immunodeficiency in a child who gets many infections or unusual infections. Testing may be done as part of an evaluation for allergies or autoimmune conditions, such as juvenile idiopathic arthritis, lupus, and celiac disease.
How should we prepare for an immunoglobulin test?
Children can eat and drink normally unless other tests that require fasting are also done. Tell your doctor about any medications your child takes, as some medications can affect the test results. Wearing a t-shirt or short-sleeved shirt to the test can make things easier for your child, and you can also bring a toy or book as a distraction.
Results:
A total of 637 participants were included in this investigation. Two employees tested positive for IgM on the CLIA quantitative antibody test (cutoff value: 10 AU/mL) out of 51 employees who tested positive for IgM on the rapid test kit. Six staff members tested positive for IgG on the CLIA quantitative antibody test out of 56 staff members who tested positive for IgG on the rapid test kit. The proportion of staff with positive antibodies differed greatly between the rapid test kit and the quantitative CLIA antibody test.
Conclusions:
There was a large difference in the proportions of staff with positive IgG and IgM antibodies in the rapid test kit and in the CLIA quantitative antibody test results. Results from the single rapid test kit may need to be interpreted with caution. Further studies are required to assess the accuracy of antibody tests to further understand the characteristics of each assay and determine its purposes in each community.
Keywords:
Prevalence of antibodies; COVID-19; Serological assay.